Stellen Sie sich vor, Ihre Hände oder Füße werden plötzlich von einem heftigen, brennenden Schmerz übermannt – so stark, als stünden sie in Flammen. Ihre Haut färbt sich leuchtend rot, schwillt an und strahlt Hitze aus, als wären Sie verbrüht worden. Doch es gibt keine sichtbare Verletzung, keine äußere Ursache. Dies ist die bittere Realität für Menschen, die mit … leben. Erythromelalgie, eine seltene und oft missverstandene Krankheit, die den Alltag in einen Kampf gegen ein unsichtbares Feuer verwandelt.
Wenn Sie oder ein Ihnen nahestehender Mensch unter diesen Symptomen leidet, sind Sie nicht allein. Dieser Ratgeber erklärt die Krankheit verständlich und bietet Ihnen klare, praktische Einblicke in die Erythromelalgie, ihre Ursachen und die wirksamsten Strategien, um wieder Linderung und Kontrolle zu erlangen. Lassen Sie uns dieses Rätsel gemeinsam lösen.

Was ist Erythromelalgie? Das Feuer in uns
Erythromelalgie ist eine seltene Gefäßerkrankung, die durch wiederkehrende Episoden gekennzeichnet ist brennender Schmerz, Rötung der Extremitätenund warme Haut. Diese Symptome treten typischerweise an Händen und Füßen auf, können aber auch Arme, Beine oder sogar das Gesicht betreffen. Häufige Auslöser sind Wärme, körperliche Anstrengung oder langes Stehen, wodurch alltägliche Tätigkeiten zu qualvollen Torturen werden.
Es gibt zwei Haupttypen von Erythromelalgie:
- Primäre Erythromelalgie: Diese Form tritt spontan auf und ist häufig mit genetischen Mutationen verbunden, die die normale Funktion kleiner Blutgefäße beeinträchtigen. Sie kann in jedem Alter auftreten, manifestiert sich aber häufig im Kindes- oder frühen Erwachsenenalter.
- Sekundäre Erythromelalgie: Diese Form entwickelt sich als Komplikation zugrundeliegender Erkrankungen wie Autoimmunerkrankungen, Nervenschädigungen oder Blutkrankheiten wie Polycythaemia vera. Die Behandlung der Ursache ist entscheidend für eine wirksame Symptomkontrolle.
Das charakteristische Merkmal der Erythromelalgie ist ihre episodischer Charakter. Die Symptome können ohne Vorwarnung auftreten, Minuten bis Tage anhalten und Betroffene oft hilflos und isoliert zurücklassen. Das Brennen ist nicht nur unangenehm, sondern ein quälender Schmerz, der Schlaf, Arbeit und den Alltag beeinträchtigen kann.
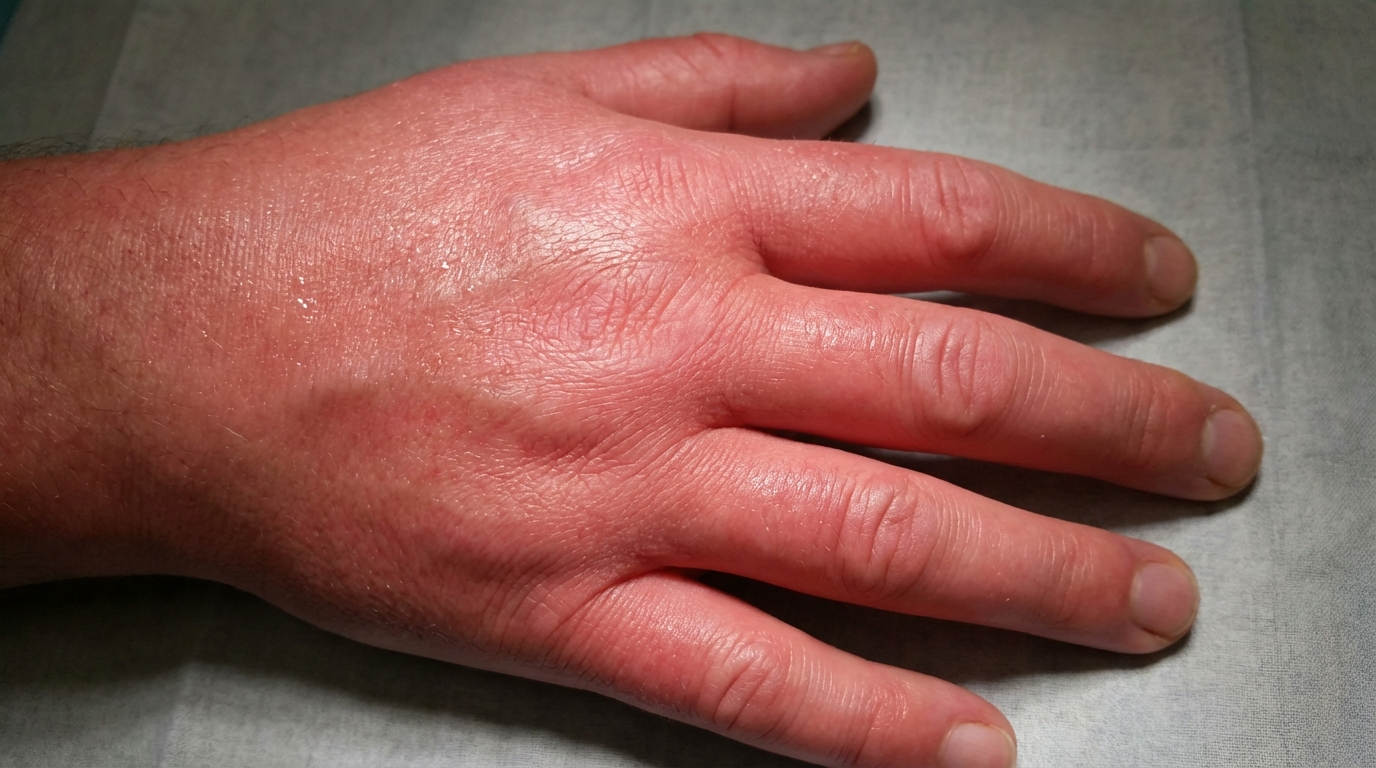
Die diagnostische Herausforderung: Warum Erythromelalgie oft missverstanden wird
Die Diagnose von Erythromelalgie stellt selbst erfahrene Kliniker vor Herausforderungen. Ihre Symptome –brennender Schmerz, Rötungund WärmeDie Symptome ähneln denen häufigerer Erkrankungen wie Neuropathie, Raynaud-Syndrom oder sogar allergischen Reaktionen. Diese Überschneidung führt oft zu Fehldiagnosen oder verzögerter Behandlung, wodurch Patienten in einem Teufelskreis aus Frustration und ungelinderten Schmerzen gefangen bleiben.
Erschwerend kommt hinzu, dass es keinen einzelnen Test für Erythromelalgie gibt. Die Diagnose beruht auf einer Kombination folgender Faktoren:
- Klinische Beurteilung: Eine detaillierte Anamnese der Symptome, einschließlich Auslöser (z. B. Hitze, körperliche Anstrengung) und Dauer der Episoden.
- Körperliche Untersuchung: Beobachtung der charakteristischen Rötung, Wärme und Schwellung während eines akuten Krankheitsschubs.
- Ausschluss anderer Bedingungen: Ausschluss alternativer Diagnosen durch Bluttests, Nervenleitstudien oder Bildgebung.
Bei Verdacht auf sekundäre Erythromelalgie ist die Identifizierung der zugrunde liegenden Ursache – wie beispielsweise einer Autoimmunerkrankung oder einer Blutdyskrasie – für die individuelle Anpassung der Behandlung unerlässlich.
Auslöser und Ursachen: Was entfacht das Feuer?
Die genaue Ursache der Erythromelalgie ist weiterhin unklar, doch Forschungsergebnisse deuten auf eine Funktionsstörung der kleinsten Blutgefäße (Kapillaren) und Nerven des Körpers hin. Diese Funktionsstörung führt zu abnormalen Blutungen. Gefäßerweiterung—eine Erweiterung der Blutgefäße—die dazu führt, dass sich Blut in den Extremitäten staut und dadurch Schmerzen und Entzündungen ausgelöst werden.
Häufige Auslöser sind:
- Hitzeeinwirkung: Warme Umgebungen, heiße Bäder oder auch nur leichte Temperaturerhöhungen können Symptome hervorrufen.
- Körperliche Aktivität: Sportliche Betätigung oder langes Stehen können aufgrund der erhöhten Durchblutung zu Krankheitsschüben führen.
- Stress und Angstzustände: Psychischer Stress kann die Symptome verschlimmern und einen Teufelskreis aus Schmerz und psychischer Belastung auslösen.
- Enges Schuhwerk oder Kleidung: Einengende Gegenstände können die Durchblutung beeinträchtigen und Beschwerden verschlimmern.
Auch genetische Faktoren spielen eine Rolle, insbesondere bei der primären Erythromelalgie. Mutationen in der SCN9A Bei einigen Familien wurden Gene identifiziert, die die Nervensignalübertragung beeinflussen, was auf eine erbliche Komponente hindeutet.
Die Flammen im Griff: Behandlungsstrategien zur Linderung
Erythromelalgie ist zwar nicht heilbar, doch eine Kombination aus Lebensstiländerungen, Medikamenten und unterstützenden Therapien kann die Symptome lindern und die Lebensqualität verbessern. Ziel ist es, Häufigkeit und Schwere der Krankheitsschübe zu reduzieren und die Beschwerden während der Episoden zu minimieren.
1. Lebensstiländerungen: Das Feuer löschen
Einfache, aber wirksame Änderungen des Lebensstils können einen bedeutenden Unterschied machen:
- Coole Umgebungen: Sorgen Sie für ein angenehmes Raumklima in Ihren Wohn- und Arbeitsräumen. Nutzen Sie Ventilatoren, Klimaanlagen oder Kühlgel, um eine komfortable Temperatur zu gewährleisten.
- Auslöser vermeiden: Meiden Sie Wärmequellen, anstrengende Aktivitäten und enge Kleidung, die die Blutzirkulation behindern könnte.
- Extremitäten hochlagern: Das Anheben der Hände oder Füße über Herzhöhe kann helfen, Blutansammlungen zu reduzieren und Symptome zu lindern.
- Flüssigkeitszufuhr: Ausreichende Flüssigkeitszufuhr fördert die Durchblutung und kann dazu beitragen, Krankheitsschübe zu lindern.
2. Medikamente: Die Ursache des Schmerzes bekämpfen
Mehrere Medikamente haben sich bei der Behandlung von Erythromelalgie-Symptomen als vielversprechend erwiesen:
- Aspirintherapie: Niedrig dosiertes Aspirin ist oft die Therapie der ersten Wahl, insbesondere bei sekundärer Erythromelalgie im Zusammenhang mit Blutkrankheiten. Es hilft, das Blut zu verdünnen und die Durchblutung zu verbessern.
- Topisches Lidocain: Das Auftragen von Lidocain-Cremes oder -Gels auf die betroffenen Stellen kann durch Betäubung vorübergehende Linderung verschaffen. Nervenschmerzen.
- Vasokonstriktoren: Medikamente, die die Blutgefäße verengen, wie beispielsweise Betablocker oder Kalziumkanalblocker, können dazu beitragen, Blutansammlungen zu reduzieren.
- Antikonvulsiva: Medikamente wie Gabapentin oder Pregabalin können bei der Behandlung chronischer Erkrankungen helfen. Nervenschmerzen im Zusammenhang mit Erythromelalgie.
Konsultieren Sie vor Beginn der Einnahme von Medikamenten immer einen Arzt, da die individuellen Reaktionen sehr unterschiedlich sein können.
3. Fortschrittliche Therapien: Neue Horizonte erkunden
Bei schweren oder therapieresistenten Fällen können weiterführende Interventionen in Betracht gezogen werden:
- Nervenblockaden: Lokalanästhetika können die Schmerzsignale in den betroffenen Nerven vorübergehend blockieren.
- Biofeedback-Therapie: Diese Technik lehrt Patienten, physiologische Reaktionen wie die Durchblutung durch mentale Strategien zu kontrollieren.
- Experimentelle Behandlungen: Neue Therapien wie Botulinumtoxin-Injektionen (Botox) werden hinsichtlich ihres Potenzials zur Linderung von Schmerzen und Entzündungen erforscht. Erfahren Sie mehr über Botox-Anwendungen im Bereich der Schmerztherapie.
Leben mit Erythromelalgie: Bewältigungsstrategien und Unterstützung
Das Leben mit Erythromelalgie ist eine tägliche Herausforderung, doch der Aufbau eines Unterstützungsnetzwerks und die Anwendung von Bewältigungsstrategien können Ihnen helfen, die Kontrolle zurückzugewinnen. So geht's:
- Informieren Sie sich: Wissen ist Macht. Wenn Sie Ihre Erkrankung und deren Auslöser verstehen, können Sie fundierte Entscheidungen über Ihre Behandlung treffen.
- Mit anderen verbinden: Online-Communities und Selbsthilfegruppen bieten einen geschützten Raum, um Erfahrungen auszutauschen und von anderen zu lernen, die ähnliche Schwierigkeiten durchmachen. Du bist auf diesem Weg nicht allein.
- Psychische Gesundheit priorisieren: Chronische Schmerzen können das seelische Wohlbefinden stark beeinträchtigen. Therapie, Achtsamkeitsübungen oder Entspannungstechniken können helfen, Stress und Angstzustände zu bewältigen.
- Zusammenarbeit mit Spezialisten: Arbeiten Sie mit einem Team aus medizinischen Fachkräften zusammen, darunter Dermatologen, Neurologen und Schmerztherapeuten, um einen umfassenden Behandlungsplan zu entwickeln. Für eine fachkundige dermatologische Betreuung sollten Sie eine Beratung in Betracht ziehen. Dr. Ebru Okyay.
Fazit: Wie Sie Ihr Leben nach der Erythromelalgie zurückgewinnen
Erythromelalgie kann sich wie ein unerbittliches Feuer anfühlen, doch mit den richtigen Strategien, Unterstützung und ärztlicher Beratung ist es möglich, die Beschwerden zu lindern und Ihr Leben zurückzugewinnen. Von Anpassungen des Lebensstils bis hin zu fortschrittlichen Therapien – jeder Schritt bringt Sie der Linderung und neuen Hoffnung näher.
Denken Sie daran: Ihre Erkrankung definiert Sie nicht. Indem Sie sich informieren, aktiv werden und sich vernetzen, können Sie die Herausforderungen der Erythromelalgie mit Stärke und Resilienz meistern. Wenn Sie bereit sind, individuelle Behandlungsmöglichkeiten zu erkunden, wenden Sie sich noch heute an einen vertrauenswürdigen Spezialisten.
Die wichtigsten Erkenntnisse
- Erythromelalgie ist eine seltene Erkrankung, die gekennzeichnet ist durch brennender Schmerz, Rötungund Wärme in den Extremitäten.
- Primäre und sekundäre Formen erfordern unterschiedliche Diagnose- und Behandlungsansätze.
- Lebensstiländerungen, Medikamente und moderne Therapien können helfen, die Symptome effektiv zu lindern.
- Der Aufbau eines Unterstützungsnetzwerks und die Priorisierung der psychischen Gesundheit sind für die langfristige Bewältigung von Problemen entscheidend.
- Die Beratung durch Spezialisten gewährleistet einen maßgeschneiderten Behandlungsplan, der Ihren individuellen Bedürfnissen gerecht wird.
Nächste Schritte
- Verfolgen Sie Ihre Symptome und Auslöser, um Muster zu erkennen und diese Ihrem Arzt mitzuteilen.
- Probieren Sie verschiedene Kühltechniken und Medikamente aus, um herauszufinden, was für Sie am besten funktioniert.
- Treten Sie Selbsthilfegruppen oder Online-Communities bei, um Erfahrungen auszutauschen und neue Erkenntnisse zu gewinnen.
- Vereinbaren Sie einen Beratungstermin mit einem Spezialisten, um auf Ihre Bedürfnisse zugeschnittene, fortschrittliche Behandlungsmöglichkeiten zu besprechen.
Häufig gestellte Fragen (FAQs)
Wie fühlt sich der Schmerz bei Erythromelalgie an?
Die Schmerzen bei Erythromelalgie werden oft als intensives Brennen beschrieben, ähnlich wie bei Verbrühungen mit heißem Wasser. Sie können von pochenden oder stechenden Schmerzen begleitet sein, sodass selbst leichte Berührungen unerträglich werden.
Ist Erythromelalgie heilbar?
Aktuell gibt es keine Heilung für Erythromelalgie, aber die Symptome können durch eine Kombination aus Lebensstiländerungen, Medikamenten und modernen Therapien wirksam behandelt werden.
Wie wird Erythromelalgie diagnostiziert?
Die Diagnose basiert auf der klinischen Untersuchung, der Anamnese und dem Ausschluss anderer Erkrankungen. Es gibt keinen einzelnen Test, aber Blutuntersuchungen und Nervenleitstudien können helfen, die zugrunde liegenden Ursachen zu identifizieren.
Welche Kühlmaßnahmen eignen sich am besten zur Behandlung von Erythromelalgie?
Zu den Kühlmaßnahmen gehören der Einsatz von Ventilatoren, Klimaanlagen, Kühlgelen und das Hochlagern der Extremitäten. Auch das Vermeiden von Hitzeeinwirkung und eine ausreichende Flüssigkeitszufuhr sind unerlässlich.
Für fachkundige Beratung und individuelle Betreuung, vertrauen Sie Dr. Ebru Okyay, ein führendes Hautarzt Sie setzt sich dafür ein, Ihnen zu optimaler Hautgesundheit und Wohlbefinden zu verhelfen. Ob Sie an Erythromelalgie oder anderen dermatologischen Problemen leiden – ihre Expertise garantiert Ihnen eine Behandlung auf höchstem Niveau. Kontaktieren Sie uns Vereinbaren Sie noch heute Ihren Beratungstermin.