Living with a skin condition that feels like a relentless, internal fire can be exhausting. If you have noticed small, firm, and dark bumps—primarily on your shins—that trigger an uncontrollable urge to scratch, you may be dealing with lichen amyloidosis. This condition is not merely a surface-level cosmetic concern; it is a complex dermatological challenge rooted in a persistent cycle of irritation and response. Understanding the underlying mechanisms of these hyperpigmented papules is the first step toward reclaiming your skin’s health and your peace of mind.
Lichen amyloidosis represents a specific form of primary localized cutaneous amyloidosis. Unlike systemic versions of the disease, this variant remains confined to the skin. It occurs when keratin proteins from damaged skin cells transform into amyloid deposits, which then settle in the uppermost layer of the dermis. This process is almost always driven by chronic scratching or friction, creating a self-perpetuating loop where the itch leads to scratching, and the scratching leads to more amyloid buildup. At the clinic of Dr. Ebru Okyay, we prioritize identifying the root cause of such persistent pruritus to provide lasting relief.

1. The Hallmark: Intensely Itchy, Hyperpigmented Papules
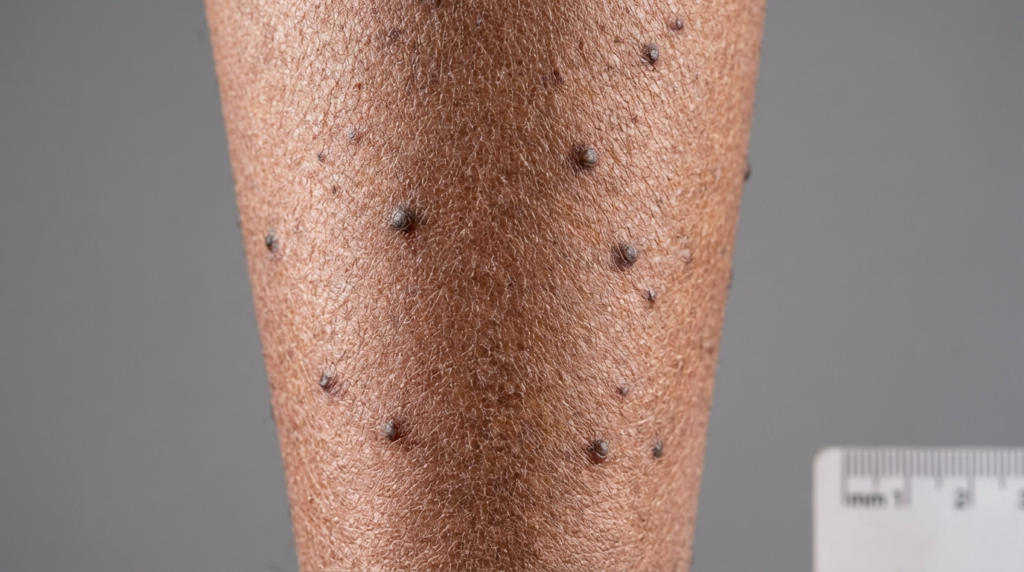
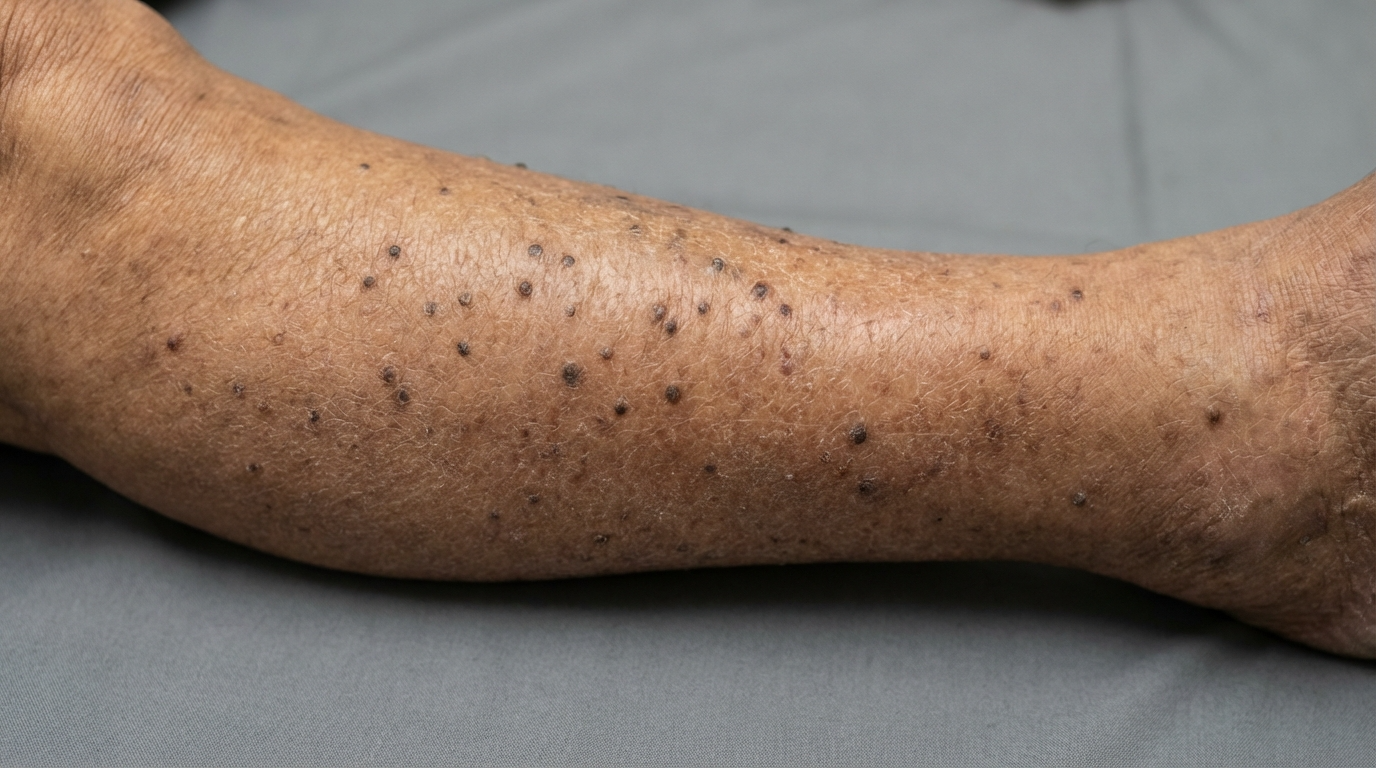
The most defining characteristic of lichen amyloidosis is the presence of intensely itchy bumps. These are typically small, scaly, and range in color from reddish-brown to greyish-brown. Because they are hyperpigmented, they often stand out significantly against the surrounding skin, leading to distress over the skin’s appearance. The texture is often described as “rippled” or “pebbly,” as the papules tend to cluster together in close proximity.
While these papules can appear on the arms or thighs, shin involvement is the most common clinical presentation. The skin over the shins is particularly susceptible to the effects of chronic scratching because it is easily accessible and has less underlying fat to cushion the impact of friction. Over time, the skin thickens—a process known as lichenification—making the area even more resistant to standard moisturizers and over-the-counter creams.
2. The Role of Chronic Scratching and Friction
Lichen amyloidosis does not appear overnight. It is the result of months or years of mechanical trauma to the skin. Whether the initial itch was caused by dry skin, a minor allergy, or stress, the repeated action of scratching causes keratinocytes (skin cells) to undergo apoptosis (cell death). The debris from these cells is then converted into amyloid, a waxy protein that the body cannot easily clear away.
This creates a biological “trap.” The amyloid deposits themselves can trigger further itching, ensuring that the patient continues to scratch. Breaking this cycle requires more than just willpower; it requires medical intervention to dampen the inflammatory response and stabilize the skin barrier. For more insights into managing complex skin conditions, you can explore our latest articles on the Dermatology Blog.
3. Why a Skin Biopsy is the Gold Standard for Diagnosis
Because lichen amyloidosis can mimic other conditions like lichen planus or chronic eczema, a definitive diagnosis is essential. A skin biopsy is the only way to confirm the presence of amyloid deposits. During this procedure, a small sample of the affected skin is removed under local anesthesia and examined under a microscope using special stains, such as Congo Red.
Under polarized light, these stains reveal a characteristic “apple-green birefringence,” which is the definitive signature of amyloid. A biopsy also allows the dermatologist to rule out systemic involvement, ensuring that the protein deposits are truly localized to the skin. This diagnostic precision ensures that the treatment plan is tailored specifically to the pathology at hand, rather than relying on guesswork.
4. Comprehensive Treatment: From Topical Steroids to Phototherapy
Managing lichen amyloidosis requires a multi-pronged approach. The primary goal is to stop the itch and reduce the visibility of the papules. Treatment usually begins with high-potency topical steroids, often applied under occlusion (covering the area with plastic wrap) to increase absorption into the thickened skin. These steroids reduce inflammation and help flatten the papules.
- Antihistamines: While they may not stop the biological cause of the itch, sedating antihistamines can help patients sleep through the night without scratching unconsciously.
- Phototherapy: Narrowband UVB light therapy has shown significant success in reducing both the itch and the size of the amyloid deposits by modulating the skin’s immune response.
- Dermabrasion: In severe or resistant cases, physical removal of the upper layers of the skin through dermabrasion can physically clear the amyloid deposits, allowing healthier skin to regenerate.
- Retinoids: Both topical and oral retinoids can help regulate skin cell turnover and prevent the further accumulation of keratin debris.
5. Long-Term Management and Prevention
Even after successful treatment, lichen amyloidosis has a high rate of recurrence if the underlying scratching habit is not addressed. Patients must adopt a “hands-off” policy. This involves keeping the skin deeply hydrated with thick emollients and avoiding harsh soaps or abrasive clothing that might trigger an itch. If you are struggling to manage a flare-up, we encourage you to contact our clinic for a personalized consultation.
Early intervention is key. The longer the condition persists, the deeper the amyloid deposits become and the more difficult they are to treat. By combining medical therapies with behavioral changes, it is possible to achieve clear skin and, more importantly, relief from the chronic discomfort that defines this condition.
Frequently Asked Questions
Is lichen amyloidosis contagious?
No, lichen amyloidosis is not an infection. It is a localized skin reaction to chronic friction and scratching; it cannot be passed from person to person.
Can lichen amyloidosis lead to internal organ damage?
Lichen amyloidosis is a primary localized cutaneous form of amyloidosis. This means it is restricted to the skin and does not affect internal organs like systemic amyloidosis does.
How long does it take to see results from treatment?
Skin healing is a slow process. While the itch may improve within weeks of starting topical steroids or phototherapy, the hyperpigmented papules may take several months to flatten and fade.
Why is the itch worse at night?
Many patients find the itch intensifies at night due to lower cortisol levels and fewer distractions, which makes the brain more sensitive to skin sensations. Sedating antihistamines are often prescribed to help with this.