Noticing dark, velvety skin patches on your body can be a source of significant anxiety. You might have tried scrubbing the area, thinking it is a matter of hygiene, only to find the discoloration persists. This condition, known medically as Acanthosis Nigricans, is far more than a cosmetic concern. It serves as a sophisticated biological “early warning system,” signaling that your internal metabolic environment requires immediate attention. In 2026, our understanding of these skin signals has evolved, allowing us to address the root causes with greater precision than ever before.
Acanthosis Nigricans typically manifests as symmetrical, hyperpigmented areas that feel thick and soft to the touch. While the visual change is striking, the underlying mechanism is often tied to how your body processes insulin. When you understand that your skin is reflecting your systemic health, you can move from frustration to proactive management. This guide provides the clarity you need to navigate this condition, offering a roadmap from diagnosis to effective treatment under the guidance of a specialist.
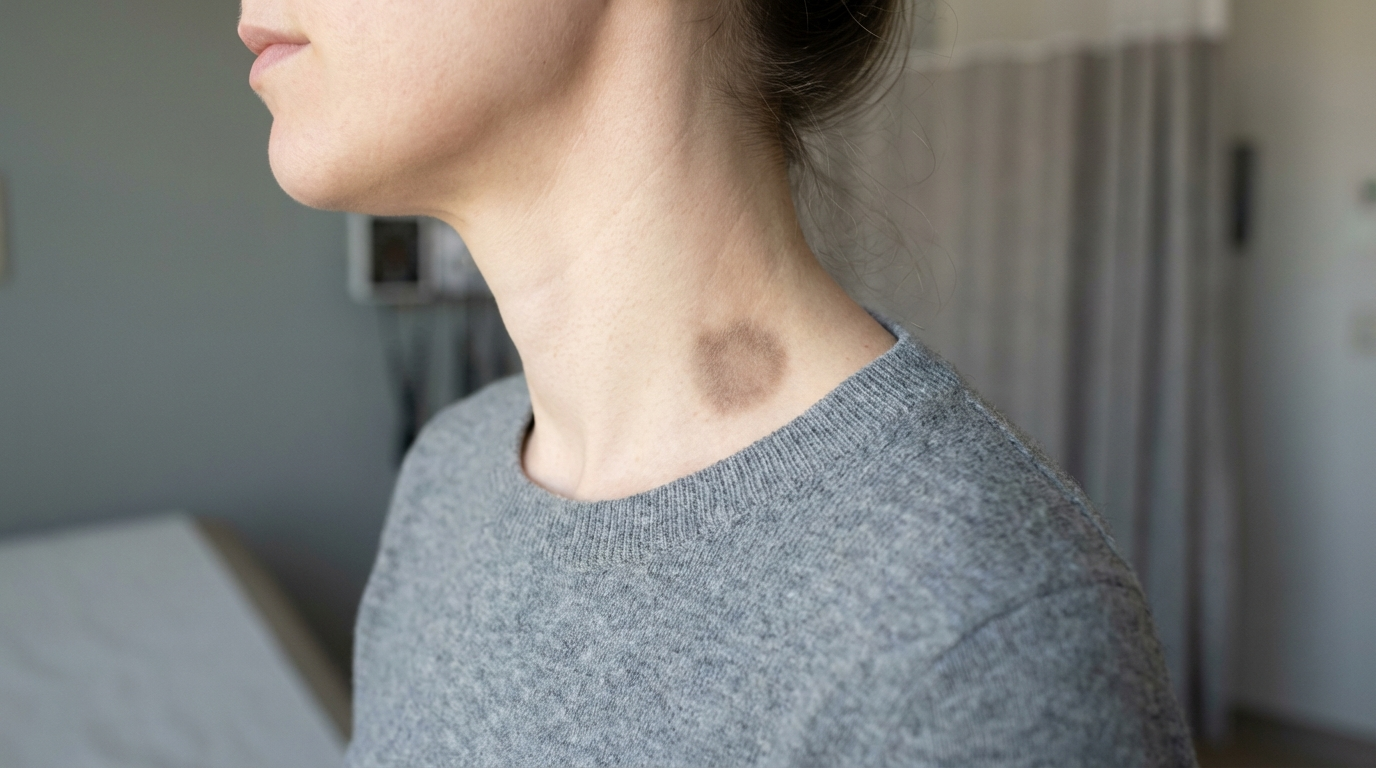
Identifying the Hallmarks of Acanthosis Nigricans
The primary characteristic of this condition is dark velvety skin. Unlike a tan or a typical bruise, these patches have a distinct texture. The skin undergoes a process called hyperkeratosis, leading to visible skin thickening. You may notice that the skin lines become more prominent, giving the area a “dirty” appearance that does not wash away.
While these patches can appear anywhere, they show a strong preference for skin folds and creases. The most common sites include:
- Neck and armpits: These are the most frequent locations for initial presentation.
- Groin and inner thighs: Friction in these areas can sometimes exacerbate the texture.
- Knuckles, elbows, and knees: Less common but indicative of more systemic involvement.
- Under the breasts: Particularly in women where moisture and friction coexist.
In most cases, the patches are asymptomatic, meaning they do not hurt. However, some patients report mild itching (pruritus) or a faint odor if the skin thickening becomes significant. Recognizing these signs early is the first step toward restoring your skin’s health and optimizing your internal well-being. For those seeking to improve overall skin texture and vitality, exploring soluzioni anti-invecchiamento can often complement medical treatments.
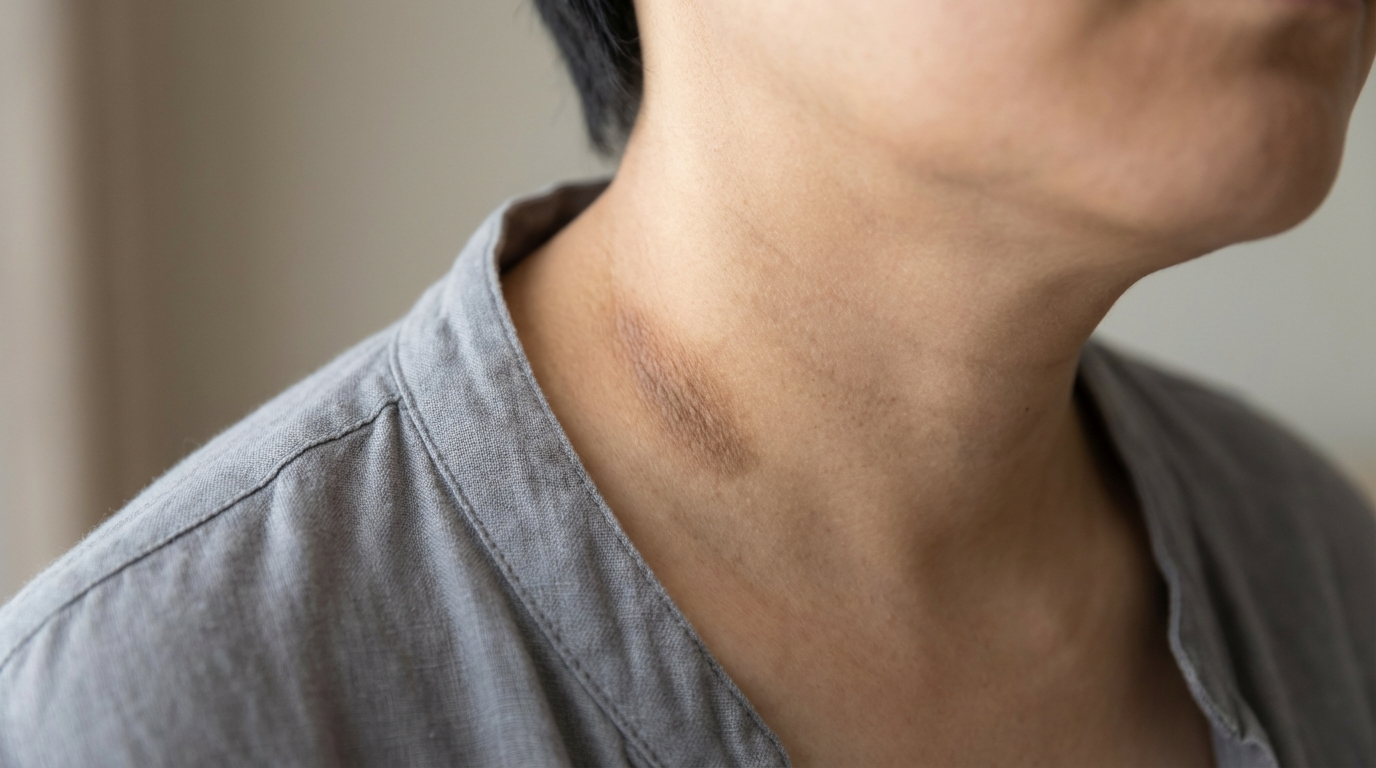
The Metabolic Connection: Why It Happens
The most critical takeaway regarding Acanthosis Nigricans is its obesity link and its role as a marker for insulin resistance. When your body’s cells become resistant to insulin, the pancreas compensates by producing more of the hormone. High levels of circulating insulin in the bloodstream spill over and bind to insulin-like growth factor receptors on skin cells (keratinocytes and fibroblasts).
This binding triggers these cells to proliferate rapidly, leading to the characteristic thickening and darkening of the skin. Consequently, this condition is frequently a precursor to or a symptom of type 2 diabetes. Addressing the skin without addressing the insulin levels is like painting over a leak; the problem will inevitably resurface.
| Categoria | Underlying Condition | Impatto sulla pelle |
|---|---|---|
| Metabolic | Insulin Resistance / Obesity | High insulin triggers skin cell overgrowth. |
| Endocrine | PCOS / Hormonal Disorders | Androgen excess contributes to skin changes. |
| Medication | Corticosteroids / Oral Contraceptives | Alters metabolic pathways and skin cell turnover. |
| Malignancy | Gastric or Liver Cancer (Rare) | Rapid onset of widespread, severe patches. |
Hormonal and Genetic Factors
Beyond insulin, various hormonal disorders can trigger these skin changes. Polycystic Ovary Syndrome (PCOS), adrenal gland disorders, and low thyroid levels are common culprits. In some instances, the condition is hereditary, appearing during childhood or puberty without any underlying systemic disease. However, a medical evaluation is always necessary to rule out metabolic complications.
When to Be Concerned: The Malignancy Association
While the vast majority of cases are benign and linked to metabolism, there is a rare form known as malignant acanthosis nigricans. This malignancy association is typically characterized by the sudden, rapid appearance of very dark and extensive patches, often involving the palms of the hands or soles of the feet. It is most commonly associated with internal cancers, such as stomach or liver adenocarcinoma.
If you notice a sudden “explosion” of these patches or if they appear in unusual places like the mouth or lips, you must seek an immediate consultation. Early detection of the underlying cause is paramount. You can contatta la nostra clinica for a comprehensive dermatological assessment to ensure your peace of mind.
Effective Treatment Strategies in 2026
The most effective treatment for Acanthosis Nigricans is treating the root cause. If weight loss and dietary changes improve insulin sensitivity, the skin patches often fade or disappear entirely without further intervention. However, we also utilize advanced topical and procedural therapies to accelerate the clearing of the skin.
Topical Interventions
To address the visible thickening and hyperpigmentation, we prescribe specific agents that encourage healthy cell turnover:
- Topical retinoids: These vitamin A derivatives help thin the thickened skin and normalize cell growth.
- Urea creams: High-concentration urea acts as a potent keratolytic, softening and dissolving the “velvety” buildup.
- Salicylic acid and Alpha-hydroxy acids (AHAs): These chemical exfoliants help remove the excess pigment trapped in the upper layers of the skin.
Clinical Procedures
For persistent or severe cases, clinical treatments can provide faster results. Chemical peels, laser therapy, and dermabrasion are effective at resurfacing the affected areas. These procedures are performed with precision to ensure that the skin heals evenly without post-inflammatory hyperpigmentation. Our team at the clinic, led by experts you can learn about on our chi siamo page, specializes in tailoring these treatments to your specific skin type.
Conclusion: Your Skin as a Guide to Health
Acanthosis Nigricans is not a permanent sentence. It is a manageable condition that often serves as a catalyst for positive lifestyle changes. By addressing the insulin resistance e obesity link, you are not just clearing your skin; you are protecting your long-term health against type 2 diabetes and cardiovascular issues. With the right combination of metabolic management and dermatological care, you can restore your skin’s natural appearance and feel confident in your own body once again.
Domande frequenti
Is Acanthosis Nigricans contagious?
No, it is not an infection and cannot be spread to others. It is a skin manifestation of internal metabolic or hormonal processes.
Can I scrub away the dark patches?
No. Scrubbing or using harsh abrasives can irritate the skin and may actually cause it to thicken further (lichenification). Treatment must focus on the underlying cause and gentle medical exfoliation.
How long does it take for the skin to return to normal?
The timeline varies. If the underlying insulin resistance is addressed through diet and exercise, you may see improvement within a few months. Topical treatments can speed up this process.
Are there specific foods I should avoid?
Since the condition is closely linked to insulin, reducing high-glycemic index foods, refined sugars, and processed carbohydrates is often recommended to improve skin symptoms.