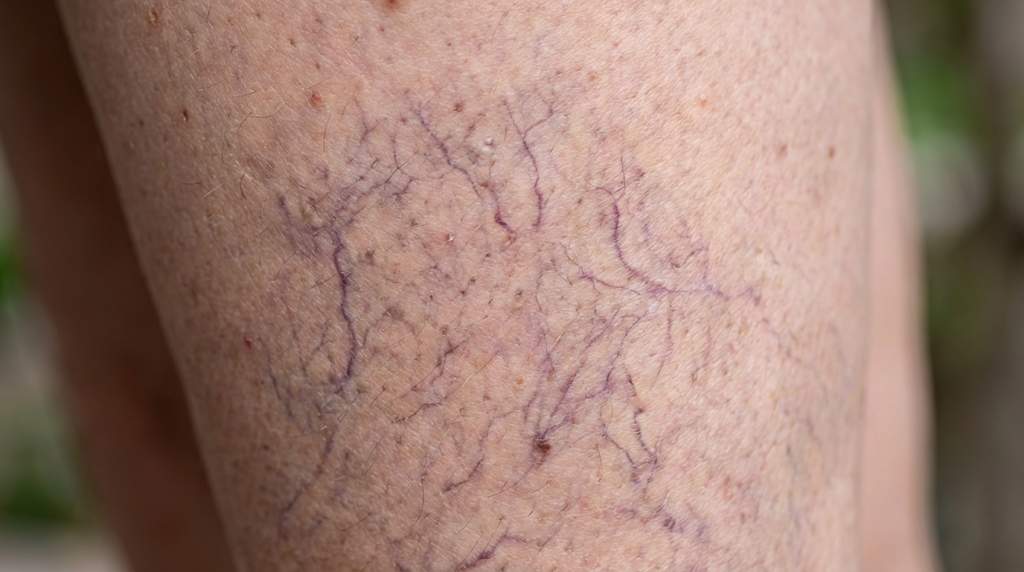
Imagine glancing at your skin and noticing a peculiar, net-like pattern—almost as if a delicate lace has been woven beneath the surface. This is livedo reticularis, a vascular phenomenon that transforms your skin into a canvas of mottled discoloration. While often harmless, its appearance can spark concern: Is it a fleeting reaction to cold, or a silent signal of something deeper?
In 2026, our understanding of livedo reticularis has evolved beyond mere observation. This guide cuts through the ambiguity, offering clear, authoritative insights into its causes, when to seek medical attention, and how to distinguish between benign patterns and those that demand further investigation. Whether you’re a patient seeking answers or a caregiver navigating this condition, you’ll leave here equipped with the knowledge to act confidently.
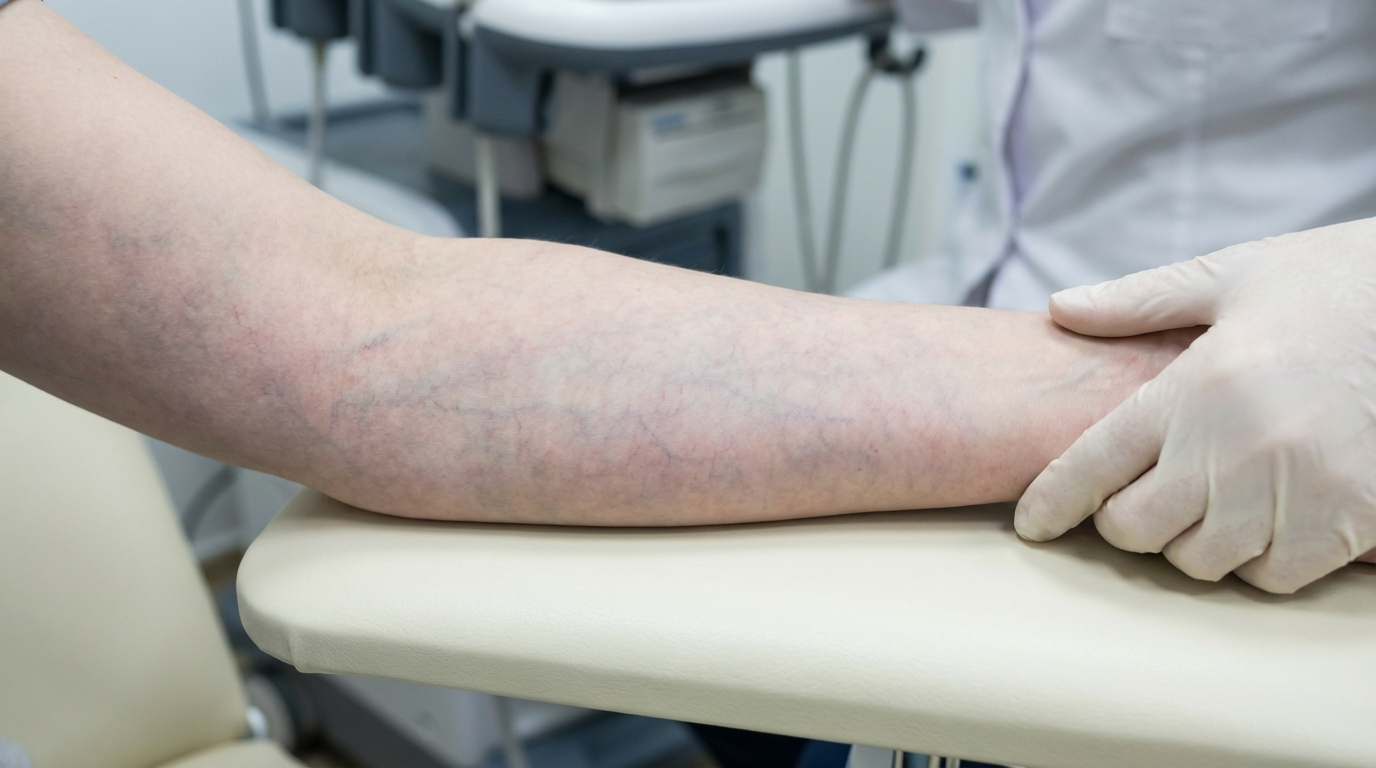
What Is Livedo Reticularis? Unraveling the Vascular Mystery
Livedo reticularis is a vascular skin condition characterized by a net-like, purplish discoloration that often appears on the legs, arms, or torso. This pattern arises from changes in blood flow within the tiny blood vessels near the skin’s surface, creating a mottled appearance. While it can be alarming, livedo reticularis is typically benign, especially when triggered by cold exposure or physiological stress.
The condition manifests due to spasms in the blood vessels or sluggish blood flow, which causes the skin to take on a blotchy, reddish-blue hue. Think of it as your body’s thermostat momentarily malfunctioning—blood pools in certain areas, while others receive less, resulting in the distinctive net-like discoloration. For most, this is a temporary and harmless reaction. However, in rare cases, it may signal an underlying disease requiring medical attention.
The Science Behind the Pattern: Blood Flow and Skin Temperature
Your skin’s appearance is intricately tied to blood flow changes. When exposed to cold, blood vessels constrict to conserve heat, sometimes unevenly. This uneven constriction creates the mottled pattern of livedo reticularis. Similarly, physiological stressors—like hormonal fluctuations or dehydration—can exacerbate the condition, making the vascular pattern more pronounced.
In 2026, dermatologists emphasize that livedo reticularis is often a benign condition, particularly when it:
- Appears symmetrically on both sides of the body.
- Fades when the skin is warmed.
- Lacks accompanying symptoms like pain, ulcers, or systemic illness.
When Livedo Reticularis Demands Attention: Red Flags and Underlying Conditions
While most cases of livedo reticularis are harmless, persistent or worsening patterns—especially when accompanied by other symptoms—may indicate an underlying disease. Conditions like Sneddon’s syndrome or antiphospholipid syndrome can manifest with livedo reticularis as a cutaneous marker. These syndromes involve abnormal blood clotting and require prompt medical evaluation.
Here’s when to act:
- Asymmetry: The pattern appears on one side of the body or in irregular patches.
- Pain or Ulcers: The skin becomes tender, or sores develop within the mottled areas.
- Systemic Symptoms: Fatigue, joint pain, or neurological issues accompany the skin changes.
- Persistence: The pattern remains visible even when the skin is warmed.
If any of these red flags are present, consult a dermatologist or rheumatologist. Early diagnosis of conditions like antiphospholipid syndrome can prevent complications such as strokes or miscarriages. For a deeper dive into vascular health, explore our Anti-Aging Solutions.

Diagnosis and Management: What to Expect in 2026
Diagnosing livedo reticularis begins with a thorough examination. Your dermatologist will assess the pattern’s distribution, symmetry, and response to warmth. In cases where an underlying disease is suspected, additional tests may include:
- Blood Tests: To check for autoimmune markers or clotting disorders.
- Skin Biopsy: Rarely needed but useful for ruling out vasculitis.
- Vascular Imaging: To evaluate blood flow in deeper vessels.
For benign cases, management focuses on lifestyle adjustments:
- Avoid Cold Exposure: Dress warmly and limit time in cold environments.
- Hydration: Maintain optimal blood flow with adequate fluid intake.
- Topical Therapies: Vasodilator creams may improve circulation in stubborn cases.
For those with Sneddon’s syndrome or antiphospholipid syndrome, treatment may involve anticoagulants or immunosuppressive therapies, tailored to the individual’s needs. Always work with a specialist to determine the best course of action.
Living with Livedo Reticularis: Reassurance and Empowerment
If your livedo reticularis is benign, rest assured: it’s a cosmetic concern, not a medical emergency. Many find comfort in knowing their vascular pattern is simply their body’s unique response to environmental triggers. However, if the pattern evolves or new symptoms arise, don’t hesitate to revisit your healthcare provider.
For those navigating more complex cases, remember: modern medicine offers robust solutions. Conditions like antiphospholipid syndrome are manageable with the right care. Your journey begins with awareness—understanding your body’s signals empowers you to take control.
Key Takeaways for Confident Action
- Benign livedo reticularis is common and often triggered by cold or stress.
- Persistent or painful patterns warrant medical evaluation for underlying conditions.
- Diagnosis may involve blood tests, biopsies, or imaging to rule out serious causes.
- Management ranges from lifestyle changes to specialized therapies, depending on the root cause.
- Empowerment starts with understanding your body and seeking expert guidance when needed.
Next Steps for Your Skin Health Journey
- Monitor your skin: Track changes in the mottled pattern and note any new symptoms.
- Consult a dermatologist: If in doubt, seek professional evaluation for peace of mind.
- Explore supportive therapies: From hydration to topical treatments, small steps can make a big difference.
Frequently Asked Questions (FAQs)
Is livedo reticularis always harmless?
While most cases are benign, livedo reticularis can sometimes indicate an underlying condition like Sneddon’s syndrome or antiphospholipid syndrome. Consult a dermatologist if the pattern persists, worsens, or is accompanied by other symptoms.
Can cold weather permanently worsen livedo reticularis?
Cold exposure typically causes temporary mottling. However, chronic exposure without protection may lead to more persistent patterns. Dressing warmly and maintaining good circulation can help minimize its appearance.
What tests are used to diagnose underlying causes of livedo reticularis?
Diagnostic tests may include blood work to check for autoimmune markers, skin biopsies to rule out vasculitis, and vascular imaging to assess blood flow. Your dermatologist will tailor the evaluation based on your symptoms.
Are there treatments to reduce the appearance of livedo reticularis?
For benign cases, lifestyle adjustments like avoiding cold and staying hydrated are often sufficient. In persistent cases, topical vasodilators or laser therapies may improve skin appearance. Always consult a specialist for personalized advice.
Dr. Ebru Okyay, a renowned dermatologist based in Antalya, specializes in diagnosing and treating complex skin conditions like livedo reticularis. Whether you’re seeking medical guidance or exploring cosmetic enhancements, Dr. Okyay’s expertise ensures personalized care tailored to your needs. Visit our About Us page to learn more about her approach or contact us to schedule a consultation.