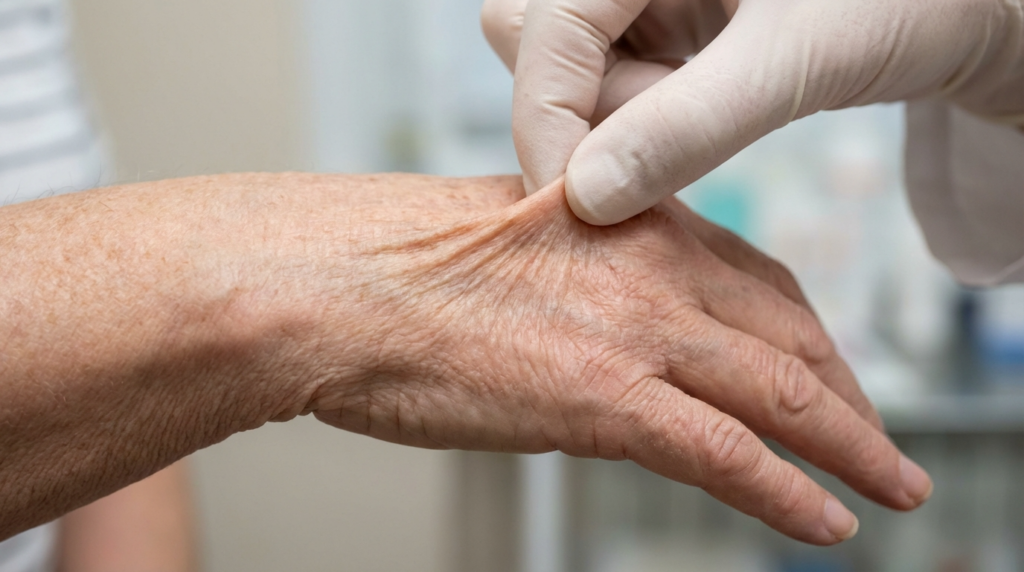
Cutis laxa represents far more than a cosmetic concern or a sign of premature aging. This rare connective tissue disorder fundamentally alters the structural integrity of the body, leading to loose, wrinkled skin that lacks the resilience found in healthy tissue. While the visual impact is often the first sign, the underlying biological mechanisms involve complex disruptions in the extracellular matrix.
In 2026, our understanding of this condition has shifted from mere observation to targeted genetic analysis. Recognizing the symptoms early is vital for managing both the dermatological and systemic manifestations. This guide provides the clarity needed to navigate the complexities of cutis laxa with confidence and medical precision.

1. The Biological Root: Elastin Fibers and Skin Elasticity
The primary culprit in cutis laxa is the degradation or absence of elastin fibers. These fibers act like biological rubber bands, allowing the skin to snap back after stretching. When these fibers fail, the skin loses its recoil, resulting in a saggy, inelastic appearance that often makes individuals appear significantly older than their chronological age.
This loss of skin elasticity is not localized. Because elastin is a critical component of connective tissue throughout the body, the disorder can affect internal organs, blood vessels, and the skeletal system. Understanding that this is a systemic issue, rather than just a surface-level problem, is the first step toward effective management.
2. Genetic Mutations and Inherited Forms
Most cases of cutis laxa stem from specific genetic mutations that dictate how the body produces and assembles connective tissue. These inherited forms are typically categorized by their mode of transmission: autosomal dominant, autosomal recessive, or X-linked. Each type carries a different prognosis and set of associated risks.
- Autosomal Dominant: Generally presents with milder systemic involvement but significant skin laxity.
- Autosomal Recessive: Often the most severe form, frequently involving internal organs and developmental delays.
- X-linked: Now often classified under Occipital Horn Syndrome, affecting copper transport and bone development.
Identifying the specific genetic marker is essential for family planning and long-term health monitoring. Modern diagnostics allow us to pinpoint these mutations with high accuracy, providing a roadmap for personalized care. For those seeking expert diagnostic support, our team at Dr. Ebru Okyay’s clinic offers specialized insights into rare skin conditions.
3. Acquired Forms: When Cutis Laxa Develops Later
Not all cases are present at birth. Acquired forms of cutis laxa can emerge in adulthood, often triggered by severe inflammatory episodes, certain medications, or autoimmune responses. In these instances, the skin may suddenly lose its firmness following a rash or a high-fever illness.
Distinguishing between genetic and acquired types is a clinical priority. Acquired cutis laxa requires a thorough investigation to rule out underlying plasma cell dyscrasias or other systemic triggers. Rapid intervention during the inflammatory phase may, in some cases, mitigate the extent of permanent skin damage.
4. Systemic Impact: Cardiovascular and Pulmonary Risks
The most serious aspects of cutis laxa occur beneath the skin. Elastin is vital for the structural health of the lungs and large arteries. Consequently, patients must be monitored for pulmonary emphysema, even in the absence of smoking, as the lung tissue loses its ability to maintain open airways.
Furthermore, cardiovascular issues such as aortic aneurysms or valve prolapse are common in severe forms. These conditions demand a multidisciplinary approach involving cardiologists and pulmonologists. Regular imaging and functional tests are mandatory to prevent life-threatening complications before they manifest symptoms.
5. Clinical Features Beyond Wrinkled Skin
While wrinkled skin is the hallmark, other clinical features provide clues to the specific subtype. Patients may exhibit a “bloodhound” facial appearance, characterized by drooping earlobes and a long philtrum. In some recessive types, joint hypermobility or skeletal abnormalities like hip dislocation are also present.
Hernias—inguinal, umbilical, or hiatal—are frequent due to the weakness of the abdominal wall and internal connective tissues. Recognizing these signs early allows for surgical planning and lifestyle adjustments that reduce strain on the body’s fragile support structures.
6. The Role of Cosmetic Surgery and Aesthetic Care
For many, the psychological impact of premature aging is profound. Cosmetic surgery, specifically rhytidectomy (facelift), can provide significant temporary improvement in appearance. However, patients must understand that because the underlying defect in elastin persists, the skin will eventually sag again.
Surgical outcomes in cutis laxa patients require specialized techniques to manage fragile tissue and ensure proper healing. While traditional anti-aging solutions may offer some support, surgical intervention remains the most effective way to address severe skin redundancy. Consultation with a surgeon familiar with connective tissue disorders is non-negotiable.
7. Multidisciplinary Management in 2026
Managing cutis laxa effectively requires a team. This team typically includes a dermatologist, a geneticist, a cardiologist, and a pulmonologist. The goal is twofold: maintaining the highest possible quality of life and preventing systemic failure. Regular screenings for vascular and respiratory health form the backbone of this strategy.
If you or a loved one are navigating the challenges of loose skin and systemic connective tissue concerns, professional guidance is available. Reach out to us through our contact page to schedule a detailed evaluation and discuss a tailored management plan.
Frequently Asked Questions
Can cutis laxa be cured?
Currently, there is no cure for the underlying genetic mutations. Management focuses on treating systemic symptoms and using surgical options to improve skin appearance.
Is cutis laxa the same as Ehlers-Danlos Syndrome?
No. While both are connective tissue disorders, Ehlers-Danlos typically involves skin hyperextensibility and joint hypermobility, whereas cutis laxa is characterized by skin that is loose and lacks recoil.
Does cutis laxa affect life expectancy?
Life expectancy depends on the subtype. Autosomal dominant forms often have a normal lifespan, while certain recessive forms with severe internal organ involvement may reduce life expectancy.
Are there non-surgical treatments for the skin?
Topical treatments and lasers have limited efficacy because the problem lies in the deep elastin fibers. Surgery remains the primary method for addressing significant skin laxity.
References
Berk, D. R., Bentley, D. D., Bayliss, S. J., Lind, A., & Urban, Z. (2024). Cutis Laxa: A Review of Genetics and Clinical Manifestations. Journal of Dermatological Science.
Mohamed, M., & Kouwenberg, D. (2025). Connective Tissue Disorders and the Extracellular Matrix. Clinical Genetics Review.
Urban, Z., & Davis, E. C. (2026). Elastin Fiber Assembly and Human Disease. Methods in Molecular Biology.